By Joe DiBella, REBC
PERMA FAIR is an indexed pricing platform designed to bring transparency, fairness, and long-term sustainability to employer-sponsored healthcare. Traditional healthcare pricing is largely driven by negotiated network contracts between large insurance carriers and hospitals. Those negotiations often result in reimbursement levels reaching 250%–400% of Medicare, which contributes significantly to rising healthcare costs for employers and plan sponsors. Because hospital services account for approximately 40%–50% of total healthcare spending, these pricing dynamics have produced cost increases that many employers and plan sponsors can no longer sustain. PERMA FAIR addresses this challenge by applying a consistent Medicare-based reimbursement methodology to paying hospital claims, creating a transparent and predictable payment structure. By replacing arbitrary negotiated pricing with a widely accepted benchmark, employers and plan sponsors can reduce medical spending by approximately 18%–25% while maintaining strong provider reimbursement and improving member benefits. The model combines advanced claim repricing technology with best-in-class third-party administrators and proactive care navigation, producing a system that is fair to hospitals, sustainable for employers, and protective of plan participants.
Healthcare costs are rising at unprecedented levels, and employer health plan budgets are under extraordinary pressure. At the same time, a new wave of fiduciary scrutiny is emerging around how employer health plans are managed. For decades, employers have carried fiduciary responsibility over retirement plans such as 401(k)s, ensuring that investment options and fees are reasonable and properly overseen. Increasingly, the same expectations are being applied to healthcare. Employers are being asked to demonstrate that reimbursement practices, vendor relationships, and plan structures are prudent, transparent, and aligned with the best interests of plan participants. In this environment, it becomes increasingly difficult to justify reimbursement levels at 250% or more of what Medicare pays without a defensible methodology.
Indexed pricing models such as PERMA FAIR provide a transparent and consistent framework that is far easier to defend from a fiduciary standpoint while simultaneously addressing the underlying cost drivers that continue to push healthcare spending higher.
Today’s healthcare system is largely dominated by large national insurance carriers often referred to as the BUCAs — Blue Cross, United, Cigna, and Aetna. These organizations assemble large numbers of covered lives and use that enrollment as leverage to negotiate reimbursement contracts with hospitals and providers. Over time this system has evolved through multiple plan designs including HMOs, PPOs, and high-deductible health plans. Yet despite these structural changes, the core challenge remains unchanged: healthcare costs continue to rise. In many commercial insurance contracts hospitals are reimbursed at levels reaching 250%–400% of Medicare, with significant annual increases layered on top of those rates. Because hospital services represent roughly 40%–50% of total healthcare spending, this reimbursement structure drives a large portion of the cost increases employers and plan sponsors experience today. Hospitals and insurers increasingly find themselves in conflict over reimbursement levels, while employers and plan sponsors are left to absorb the financial consequences.
PERMA FAIR approaches healthcare pricing differently. Instead of relying on arbitrary negotiated network discounts, the platform uses the Medicare fee schedule as the foundation for hospital reimbursement. Medicare is the most widely accepted reimbursement benchmark in the United States. The schedule accounts for procedure complexity, geographic variation, and regional cost differences. Under the PERMA FAIR indexed pricing approach, hospitals are typically reimbursed between 140% and 160% of Medicare. This methodology provides consistent, transparent, and predictable reimbursement while allowing employers and plan sponsors to significantly reduce overall healthcare spending. Hospitals continue to receive fair compensation, employers gain financial sustainability, and the system benefits from a pricing structure that is grounded in an objective and widely accepted benchmark.
The PERMA FAIR model operates in partnership with leading national third-party administrators. Because indexed pricing disintermediates the traditional network negotiation model, it generally does not align with the structure used by large national carriers whose business model depends on negotiating network discounts. Instead, PERMA FAIR partners with best-in-class TPAs that administer self-funded health plans. These organizations handle claims payment, member services, enrollment, eligibility, ID cards, reporting, and account management. From the member and employer perspective the experience looks identical to any other health plan. PERMA FAIR functions as the pricing engine behind the plan, ingesting Medicare data and applying proprietary algorithms to reprice hospital claims before sending those claims back to the TPA for processing and payment. In many ways PERMA FAIR serves as the “intel inside” of the health plan.
Today PERMA FAIR partners with national TPAs including AmeriHealth Administrators, Centivo, and Lucent Health, each of which brings brand credibility and deep experience administering self-funded health plans.
Under the FAIR Health Plan (the name of the member product), the participant experience remains simple and familiar. Members receive an ID card from the TPA and access care in much the same way they do today. However, the plan introduces a key advantage: members are not restricted by hospital networks. Participants may seek care at any hospital they choose. Because the plan pays hospitals using a transparent Medicare-based reimbursement schedule, there is no confusion around in-network or out-of-network status. Physician care is supported through large national PPO networks such as First Health, MagnaCare, and Prime, although members are not restricted to those providers. Most hospital services are paid at 100% of the indexed fee schedule, and physician visits generally involve only modest co-payments, allowing employees to access care with fewer financial barriers. As a result, many participants experience a plan that provides greater freedom of choice and fewer administrative hurdles than traditional network-based health plans.
The financial impact of indexed pricing is straightforward. If hospital reimbursement levels averaging approximately 250% and more of Medicare are reduced to a range of 140%–160% of Medicare, and hospitals represent roughly half of healthcare spending, the resulting savings become mathematically predictable. For many employers, the reduction in overall medical spending falls within the range of 18%–25%, depending on the organization’s claims distribution. Because the Medicare fee schedule increases gradually and predictably over time, this structure also creates a long-term mechanism for managing future healthcare cost growth. The savings generated by the model can be reinvested into stronger benefit designs while simultaneously reducing employer healthcare budgets. Importantly, these savings are not generated by shifting costs to employees through higher deductibles or increased contributions. Instead, they are achieved by applying a fair, transparent, and methodologically grounded payment approach to hospital reimbursement.
One common concern regarding indexed pricing involves billing. If a provider attempts to bill a member for the difference between the indexed reimbursement and the provider’s billed charge, the FAIR Health Plan provides immediate protection. Any bill is routed directly to the TPA and in turn the PERMA FAIR team, who then engage with the provider to resolve the issue. Providers are informed of the reimbursement methodology and asked to work directly with the plan rather than the member. In most situations these issues are resolved collaboratively. When necessary, ERISA protections support the plan’s authority to determine reasonable reimbursement levels. Throughout the process members are protected and held harmless from financial exposure.
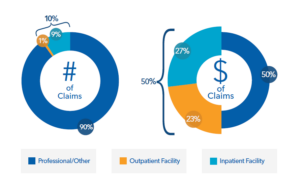
Traditional health plans often rely on complex prior authorization systems that delay care and create administrative friction for both providers and patients. The PERMA FAIR model takes a different approach. Rather than placing unnecessary barriers in front of care, the focus is on the individuals who drive the majority of healthcare spending. Approximately 10% of plan members account for nearly 90% of healthcare costs. By identifying those individuals early and surrounding them with clinical support and care navigation resources, employers can improve outcomes while controlling costs more effectively. Doctors and hospitals remain focused on delivering care, while the plan focuses on managing the overall healthcare program and ensuring that the right support is delivered to the members who need it most.
Many indexed pricing vendors that do what PERMA FAIR does charge fees based on a percentage of billed charges or calculated savings. Because billed charges often bear little relationship to the true cost of care, this approach can create misaligned incentives. PERMA FAIR instead charges a simple, transparent per-employee-per-month administrative fee. The fee is predictable, budget-able, and often one-third to one-half the cost of competing models. Because the fee is treated as an administrative expense rather than a claim expense, it also helps reduce stop-loss exposure for employers. The structure aligns incentives, maintains transparency, and ensures that employers clearly understand the cost of the services being provided.
PERMA FAIR represents a modern approach to healthcare pricing that aligns fair provider reimbursement with long-term affordability for employers and plan sponsors and better access for patients. By combining indexed pricing, best-in-class plan administration, proactive care management, and transparent fee structures, the model provides a sustainable framework for employer-sponsored healthcare. As healthcare costs continue to rise and fiduciary scrutiny increases, transparent methodologies such as PERMA FAIR offer a practical path forward for employers seeking to manage healthcare responsibly while protecting the interests of their employees.

Executive Partner, Co-President
More than 33 years of employee benefits experience
Previously led national and large account business for Horizon Blue Cross Blue Shield of New Jersey